
OUR SERVICES
THYROID SURGERY
THYROID SURGERY
Dr John Chaplin – Head and Neck Specialist Auckland NZ
Thyroidectomy Auckland New Zealand
In order to understand the need for thyroid surgery I am providing a description of the anatomy and conditions affecting the gland.
ANATOMY AND FUNCTION OF THE THYROID
The thyroid gland is a small organ in the midline of the neck, just below the Adam’s apple. It consists of a right and left lobe joined across the front of the trachea (windpipe) by a narrow bridge of thyroid tissue called the isthmus.
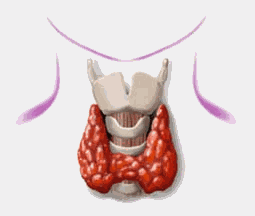
The thyroid gland makes a hormone called thyroxine, the gland requires a small amount of iodine in the diet to produce thyroxine. Because New Zealand soil is deficient in iodine it is put into our table salt. A normal amount of thyroxine is required for normal physical and mental development. All newborn babies in New Zealand are screened at birth for the presence of possible thyroid hormone deficiency.
In adults, thyroxine keeps cells and tissues working at just the right metabolic rate.
HYPERTHYROID
Too much thyroxine put out by an overactive thyroid causes an illness with a high metabolic rate called hyperthyroidism. The symptoms of this condition include tremor, heat intolerance, irritability, increased energy, poor sleep, weight loss and frequently bulging eyes. A common cause of hyperthyroidism is Grave’s Disease, an autoimmune disorder in which your immune system attacks your thyroid and causes it to make too much hormone.
Hyperthyroidism can be treated in three different ways: Firstly, drugs to block the release and effects of the hormone can be used. Secondly, it can be treated by radioactive iodine, which is taken up by the thyroid and destroys the gland. Lastly, surgical removal of the thyroid is increasingly frequently performed to treat this condition.
HYPOTHYROID
Too little thyroxine from an under-active gland causes an illness with a low metabolic rate called hypothyroidism. This condition causes tiredness, weight gain, swelling and slowness of speech and thinking. A simple blood test to measure the level of thyroxine in the blood is used to diagnose these conditions. Hypothyroidism is simply treated by taking thyroxine tablets once a day.
THYROID LUMPS AND NODULES
Enlargement of the thyroid gland is called Goitre. The entire gland may be involved or there may be single or multiple nodules or lumps.
Goitres can become very large and cause pressure on the windpipe (trachea) and swallowing tube (oesophagus). This can result in shortness of breath, voice change, cough, increased pressure sensation in the neck and sometimes difficulty swallowing.
Surgery to remove the thyroid gland is usually necessary to treat large goitres that are causing symptoms. Surgery is also necessary where there is a suspicion of thyroid cancer in an enlarged thyroid gland and where the swelling is causing cosmetic deformity. See Thyroid nodules: All you need to know.
SINGLE NODULE

A single swelling or lump (nodule) in the thyroid gland is a special form of goitre. The majority (90%) of the nodules are not cancerous but either simple swellings of fluid (cysts) or benign growths of thyroid tissue with no tendency to spread or invade structures.
The remaining 10 percent are usually a very low-grade form of cancer, which is almost always completely curable. There are a very small number of nodules that turn out to be a more aggressive form of thyroid cancer, these occur in special situations and are very rare.
Frequently the lumps are not single but multiple and part of an innocent, non-cancerous condition called multinodular goitre, which just means that several nodules are present. Multinodular goitre is the condition that causes generalised enlargement of the thyroid and can lead to compression.
CYST

Cysts ( fluid collections) in the thyroid are common. Frequently they are present without the patient noticing but sometimes they can enlarge so that they can be felt. Cysts can be diagnosed by ultrasound or by needle aspiration. Common practice is to use needle aspiration to empty the cysts of fluid. Sometimes doing this once is enough to make the cyst disappear. The aspiration may be repeated if the cyst returns; however, if the cyst returns after two or more attempts at aspiration, removing the thyroid lobe may be necessary. Radiofrequency ablation (RFA) is also increasingly used to treat benign nodules and cysts. If John thinks this is an appropriate technique for you he will refer you to an expert radiologist who has experience in this procedure.
COLLOID NODULES
These are benign nodules made up of thyroid tissue that has become enlarged. They can be single or multiple and can sometimes become very large. They can generally be diagnosed on needle biopsy; however, sometimes they can look similar to thyroid cancers on FNA, and surgical removal may be recommended. Surgery or RFA may also also necessary if the nodule becomes large and causes compressive symptoms or if they cause cosmetic deformity. Sometimes the nodules can be overactive; these will appear ‘hot’ on scintiscan and can cause hyperthyroidism.
THYROID TUMOURS
NON-CANCEROUS TUMOURS (ADENOMAS)
These tumours are caused by an abnormal growth of thyroid follicle cells. They have no capacity to spread or cause destruction of tissue but follicular adenomas cannot be differentiated from follicular thyroid cancer on FNA. Surgery is usually recommended for diagnosis. Occasionally molecular testing on repeat FNA can be used to determine the risk of malignancy. The lobe of the thyroid that has the nodule in it is removed and then examined at the laboratory to determine whether it is cancerous. Even if the nodule is proven to be malignant, often the lobectomy is all that is necessary to treat the cancer however, occasionally there is a high risk of recurrence and a completion thyroidectomy is recommended at a separate operation.
THYROID CANCER

The most common thyroid cancers are differentiated thyroid cancers and are either papillary or follicular cancer. These make up more than 90% of thyroid cancer and they very rarely cause death. They do have the potential to spread to lymph nodes in the neck and to other parts of the body such as the lungs but even if they do these tumours are still treatable.
There are some rare and more aggressive thyroid cancers which have a tendency to spread to lymph nodes in the neck and other parts of the body. One of these is medullary cancer, of which around 25% of the time occurs as part of a syndrome of hormonal tumours and is a genetic disease. Then there is poorly differentiated Cancer and high grade differentiated thyroid cancer but the most aggressive thyroid cancer is anaplastic cancer, which occurs in older patients, is very aggressive and is often untreatable. See different types of thyroid cancer at https://www.thyroid.co.nz/post/types-of-thyroid-cancer-an-update-2026
Surgery is the recommended initial treatment for virtually all thyroid cancer, and the stage and type determines whether the whole thyroid or only part of the gland should be removed. If the cancer has been noted to spread to lymph nodes or if the diagnosis is medullary cancer, the lymph nodes in the neck may be removed simultaneously in an operation called a neck dissection.
In differentiated thyroid cancer, radioactive iodine is sometimes used following surgery to kill small amounts of thyroid tumour that may have spread to lymph nodes or other areas of the body. The radioactive iodine is taken as a drink. It has very few side effects, but because you become radioactive for a short period, your doctor may advise you to keep your distance from others for a short period or even stay in hospital for 2- 3 days.
DIAGNOSIS
If you have been referred for diagnosis of a thyroid lump after an initial examination by a your GP, you may be assessed by one or more of the following methods:
BLOOD TESTS
TSH, FT4 and FT3 levels are essential to determine the function of the gland. Thyroid antibody and thyroglobulin levels are also sometimes indicated.
ULTRASOUND SCAN
This is an essential test required to measure the shape of the thyroid and to look for nodules or cysts within the gland. It is a safe and painless test that uses the principle of echoes to assess internal tissues and especially whether tissues are solid or fluid (cystic). The TIRADS (Thyroid Imaging Reporting and Data System) is used to score nodules based on their features. This system scores nodules on their ultrasound characteristics and rates them from 1-5 with the scale going from low to high risk.
FINE NEEDLE ASPIRATION BIOPSY (FNA)
This is an extremely valuable test for diagnosing thyroid lumps. A small sample of cells or fluid is removed from a thyroid nodule by passing a needle through the nodule or cyst in the gland. The aspirate is then examined under the microscope, and the type of cells making up the swelling can be seen. The test is usually very accurate. FNA causes about the same amount of discomfort as a regular blood test. Side effects are rare and are usually limited to slight discomfort on swallowing for 24 hours and trivial bruising of the skin. The Bethesda System that is used to classify the FNA biopsy and provide a risk of malignancy of the nodule. The system gives score from 1-6, again, from low to high risk and importantly there are 2 indeterminate categories, Bethesda 3 and 4. These carry risks of malignancy of 22% and 30% respectively.
CT SCAN
A cross-sectional scan will be necessary if there is recurrent goitre, thyroid cancer with involved lymph nodes or a large retrosternal thyroid causing compression. CT is not usually indicated for smaller palpable thyroid lumps as ultrasound gives much more information regarding the structure of a nodule and its risk of malignancy.
MOLECULAR TESTING
Nodules that have been shown to have indeterminate cytology Bethesda 3 or 4 may be further risk stratified by having molecular studies performed on cells from the needle aspirate. This is becoming increasingly recommended and there are commercial tests that are available that Dr John Chaplin will discuss with you if appropriate. John favours and recommends the Thyroseq V3 Genomic Classifier test and has used this test for several years now.
THYROID SURGERY (THYROIDECTOMY)
TOTAL THYROIDECTOMY

If the decision has been made to surgically treat your thyroid condition, John will explain that it may be necessary to remove all or only part of the gland. Total thyroidectomy is usually indicated when a nodule is definitely known to be cancerous on FNA and when there are indications for post-operative radioactive iodine, i.e. if the tumour is >4cm in size (T3a), or if it is any size and has obvious extra-thyroid extension (T3a), or there are clinically involved lymph nodes (T+N1). Total thyroidectomy is also indicated when the entire gland is enlarged and causing compression and in Graves Thyrotoxicosis. Following a total thyroidectomy, you will need to take thyroxine tablets every day to replace the hormone that the thyroid produces.
HEMI-THYROIDECTOMY (THYROID LOBECTOMY)
When a nodule is only suspicious of cancer on FNA, or a diagnosed thyroid cancer is <2 cm (T1)or is <4cm (T2) without extension outside the gland and/or there are no involved nodes, Dr Chaplin may recommend having a hemi-thyroidectomy (thyroid lobectomy), i.e. removal of the half of the gland that contains the nodule or tumour. Sometimes, a pathologist will examine the nodule or sampled neck lymph nodes while you are still under the anaesthetic and decide whether the remaining half of the gland needs to be removed. Benign conditions affecting one lobe of the gland may also be treated by thyroid lobectomy, e.g. if there is hyperthyroidism from a one-sided toxic nodule or compression from an enlarged benign nodule. Thyroxine is usually not necessary following removal of half the gland.
SUBTOTAL-THYROIDECTOMY
This is uncommonly performed now but in the past in cases where Graves hyperthyroidism was being treated by surgery, sometimes about three quarters of the gland was removed and a portion was left behind to continue to function. Because of the unpredictability of the correct portion to leave behind and the risk of persistent hyper-thyroidism or hypo-thyroidism, total thyroidectomy is usually recommended in this condition.
NECK DISSECTION
During investigation for thyroid cancer, lymph nodes either in the central or lateral neck are examined and often biopsied to determine whether they may be involved with metastatic thyroid cancer. In certain tumours nodes are frequently involved. If there is clinical, radiological and pathological evidence of lymph node involvement, those nodes will need to be removed at the time of your surgery. This part of the operation is called a Neck Dissection and it will either target the central or lateral neck. The central neck is accessed through a typical thyroidectomy scar but a lateral neck dissection needs an extended scar that usually runs from the thyroid scar horizontally in the neck. This incision usually results in some numbness that can persist for life but usually settles. Numbness related to the thyroid scar is less common.
PROCEDURE
Thyroid surgery is performed under general anaesthesia through a horizontal incision in a skin crease in the front of the neck. The incision can vary in length depending on the size of the thyroid gland. The wound is carefully closed at the end of the procedure, and most of the time, the scar is very cosmetically acceptable in the mid to long term ( months to years).
COMPLICATIONS
Your surgeon John will explain the risks of the operation to you. It is important to note that these complications are rare, they include:
Nerve injury
Two nerves that are close to the thyroid gland on each side that allow the larynx (voice-box) to function. If these nerves, called the recurrent laryngeal nerve (RLN) and the external branch of superior laryngeal nerve (EBSLN), are injured during thyroid surgery the character of your voice may change. This is very uncommon particularly in an experienced surgeons hands and any change at all is usually temporary. Inraoperative nerve monitoring (IONM) is used with an electrode on the tube that sits in the windpipe between the vocal cords used to keep you oxygenated during surgery. The nerves can be stimulated and signals will be recorded on the electrode. This offers information about the electrical integrity of the nerves that adds to the visual information of seeing an intact nerve.
Low Calcium Levels
During a total thyroidectomy there is a risk of injuring the para-thyroid glands. These four small glands are attached to the back of the thyroid gland and help to control the body’s calcium level. If these are injured the calcium levels in your blood can fall. Calcium is important for nerve and muscle function and you may need to take calcium tablets if this happens. If this happens at all it is usually a temporary problem and the glands usually start to function again after a period.
Bleeding
As with any surgery bleeding can sometimes occur after the operation. If this happens your neck may swell and you may have to be taken back to the operating room to have the blood drained away.
Pain
Thyroidectomy is not usually a painful operation, there may be some minor discomfort with swallowing and neck movement following surgery for a short time. Simple pain relieving medications are very effective.
One to two days will be needed in hospital following this operation. Blood calcium levels may be checked during your stay. A drain may be placed into the wound at the time of surgery, this is usually removed after one or two days. About a week is required to recover before resuming normal activities.